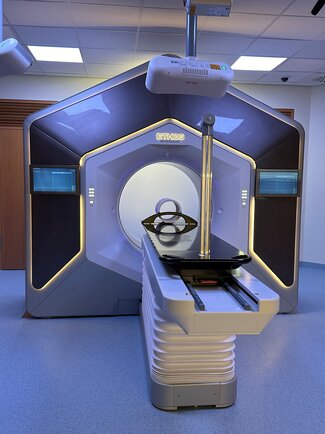
Radiation Therapy
Radiation therapy, also known as radiation oncology, radiotherapy, or radiological medicine, involves the medical use of ionizing radiation. Its goal is to cure diseases—particularly malignant tumors, but also benign ones—to slow their progression, or to alleviate symptoms.
Alongside surgery and drug therapy, radiation therapy plays a crucial role in the treatment of cancer. It can be used as the sole treatment for a tumor or administered before, during, or after surgery. Additionally, radiation therapy can be combined with anti-tumor drugs.
In this context, radiation-sensitizing substances can be administered during chemotherapy or immunotherapy to make the tumor tissue even more sensitive to radiation. To better protect healthy tissue, radiation-protective substances can also be applied. Which treatment is the right one depends on the specific case and is determined in an individualized treatment plan.
Depending on the type of cancer, radiation therapy is used curatively or palliatively. In curative treatment, the goal is to completely destroy the tumor. If this is successful, the patient is cured. It may therefore also be advisable to administer preventive radiation, for example after surgery, to destroy any individual tumor cells that may have remained in the surgical area. When a cure for a tumor is no longer possible—for example, if metastases are already present—palliative radiation therapy ensures that symptoms such as pain, shortness of breath, bleeding, or paralysis are alleviated or even prevented. This significantly improves the well-being and quality of life of the cancer patient.
Two basic procedures are used in radiation therapy: percutaneous radiation therapy and brachytherapy.
Percutaneous radiation therapy
Percutaneous radiation therapy is a highly precise form of external beam radiation therapy in which radiation is directed at the tumor from outside the body. Using state-of-the-art imaging and computer-controlled radiation techniques—such as intensity-modulated radiation therapy (IMRT) and image-guided radiation therapy (IGRT)—the affected tissue is treated with millimeter precision.
This proven and effective method is used for a wide range of tumor diseases, often in combination with surgery or drug therapies. The major advantage of percutaneous radiation therapy is that the radiation can be precisely adapted to the shape of the tumor, enabling effective treatment while simultaneously minimizing damage to the surrounding healthy tissue.
Brachytherapy
Brachytherapy is an extremely precise form of internal radiation therapy in which a tiny radioactive source is placed directly in or on the tumor. Using state-of-the-art imaging (ultrasound, CT, or MRI) and computer-controlled applicators or thin hollow needles—under anesthesia if necessary to ensure a pain-free procedure—the affected tissue is irradiated with millimeter precision. This effective method is used particularly for prostate, uterine, breast, and skin cancer, often in combination with external radiation therapy or chemotherapy. The major advantage of brachytherapy is that the radiation has a very short range, allowing the tumor to be targeted with an extremely high dose while simultaneously sparing the surrounding healthy tissue as much as possible. This enables excellent chances of cure with good tolerability.
-
1Determining the Treatment Plan
For each individual patient, a personalized treatment plan is developed during so-called tumor board meetings, which are attended by specialists from various disciplines, including surgeons, internists, pathologists, radiologists, nuclear medicine specialists, psycho-oncologists, and palliative care specialists. -
2Patient Information
During a detailed consultation, the radiation oncologist explains to the patient whether radiation therapy will be used as the sole treatment in their case or whether it will be administered in combination with radiation-sensitizing agents (radiochemotherapy, immunotherapy) and/or radiation-protective agents. -
3Preparing the Patient for Radiation Therapy
Special positioning systems are used to ensure the patient is positioned optimally on the treatment table. This position is not changed during treatment to ensure that the same area is always irradiated. To this end, special positioning aids or mask systems are fabricated in the Medical Physics Engineering Laboratory. -
4Imaging for Radiation Therapy Planning
Various imaging methods are used to create radiation treatment plans, such as computed tomography (CT), magnetic resonance imaging (MRI), and positron emission tomography (PET). This is done with the patient positioned exactly as they will be during the actual radiation treatment. Using the image data obtained in this way, the radiation oncologist can clearly distinguish tumors from healthy tissue when planning the treatment. -
5Radiation Therapy Planning
When planning radiation therapy, the physician and medical physicist work closely together. The radiation oncologist determines the target volume to be irradiated and marks it, along with the organs at risk, on the CT images. The oncologist also specifies where each radiation dose should be delivered. A medical physicist then calculates the dose distribution. Finally, the plan is evaluated jointly by the physician and the medical physicist: only once both have accepted and approved the plan can the patient receive radiation therapy. -
6Radiation Therapy
During radiation therapy, medical technologists in radiology (MTR) assist in the care of patients. Their role is to prepare patients for radiation therapy and to operate the linear accelerator. In doing so, they work closely with physicians, physicists, and staff from the Medical Physics Engineering Laboratory. The actual treatment is over quickly: depending on the treatment plan, it lasts from just a few seconds to a few minutes. -
7Monitoring During Radiation Therapy
During radiation therapy, the accuracy of the radiation delivery is regularly monitored at the treatment machine using imaging techniques such as CT scans or X-rays. This allows for the precise detection of the location of tumors that move due to factors such as breathing or the heartbeat, and enables the patient’s positioning to be adjusted accordingly. -
8Consultations with the doctor during treatment
Regular consultations with the doctor take place during radiation therapy. Patients can also contact their radiation oncologist at any time if they have questions or concerns. -
9Completion of Radiation Therapy
Once radiation therapy is complete, a detailed follow-up consultation with the treating physician takes place. During this consultation, it is determined, among other things, whether the treatment is now complete or whether further therapeutic measures are necessary. -
10Follow-up Examinations
About 6 to 8 weeks after the end of radiation therapy, the patient returns to the clinic for their first follow-up appointment. A physician conducts a thorough examination to determine how the radiation treatment has worked and whether the tumor is under control or has been cured. The physician also checks for any side effects or long-term effects so that appropriate measures can be taken. The follow-up care required by law lasts for several years and takes place in close collaboration with the respective specialists and primary care physicians who care for the patients at home.
Range of treatments
- Radiation Therapy for Cancer
- Brain tumors
- ENT tumors
- Breast cancer
- Lung cancer
- Gastrointestinal tumors
- Prostate cancer
- Gynecological tumors
- Sarcomas
- Lymphomas
- Dermatological tumors
- Pediatric tumors
- Radiation therapy for inflammatory joint diseases
Technology
- IMRT (Intensity-Modulated Radiation Therapy)
- IGRT (Image-Guided Radiation Therapy)
- Stereotactic Body Radiation Therapy (SBRT) and Stereotactic Ablative Brain Radiation Therapy (SABR)
- Adaptive radiation therapy
- Breath holding (DIBH, abdominal compression)
- Brachytherapy and IORT (Interventional Radiology Section)
- Hyperthermia
- BrainLab
- ExacTrac
- C-arm
- Stereotaxy for brain metastases (SRS, stereotaxy)
_____________________
Our digital resource on prostate cancer provides you with scientifically sound information from the Uniklinik Freiburg on prostate cancer and radiation therapy. We welcome your feedback.