Research Group „Human T-cell immunodeficiency“
Prof. Dr. Stephan EhlThe research group „Human T-cell immunodeficiency“ works at the interface of clinical and basic research with a focus on human T cell immunity. The research projects encompass the whole spectrum of translational research from the identification and characterization of novel gene defects followed by pathophysiological studies in mouse models and human patients to the development of novel diagnostic tools and using this basic knowledge in the design of international treatment trials.
CV
| seit 2020 | Gewähltes Mitglied der Nationalen Akademie der Wissenschaften (Leopoldina) |
| seit 2018 | Direktor des Instituts für Immundefizienz am Universitätsklinikum Freiburg |
| seit 2015 | Sprecher SFB1160 "IMPATH" |
| seit 2012 | Medizinischer Direktor des Centrum für Chronische Immundefizienz |
| 2008-2012 | Wissenschaftlicher Direktor des Centrum für Chronische Immundefizienz |
| 2003 | Habilitation in Pädiatrie |
| seit 2002 | Oberarzt, Universitäts-Kinderklinik Freiburg |
| 1998-2002 | Assistenzarzt, Universitäts-Kinderklinik Freiburg |
| 1995-1997 | Post-Doc, Institut für Experimentelle Immunologie, Universität Zürich |
| 1994-1995 | Postgraduate Course für Experimentelle Medizin und Biologie, Universität Zürich |
| 1993-1994 | Assistenzarzt, Universitäts-Kinderklinik Ulm |
| 1985-1991 | Medizinstudium in Aachen, Erlangen und München |
Research Areas
T cell immunity is important for the control of most infections. A successful T cell response involves antigen recognition, cellular activation and differentiation, rapid expansion and exertion of eff ector functions. These potent and highly dynamic processes must be tightly regulated in order to avoid inappropriate or uncontrolled infl ammatory responses. Human genetic diseases provide a fascinating window to understand T cell immunity and its relevance for the control of infectious diseases as well as for diseases of immune dysregulation.
The research group „Genetic deficiencies of human T cell immunity“ works at the interface between clinical and basic immunology with a particular focus on T cell immunity. The research activities cover a large spectrum from basic research in animal models or the identifi cation of new genetic defects to international diagnostic and clinical studies. The group integrates both physicians and basic scientists.
We study three immunodeficiency states representing models for different aspects of T cell immunity:
Summary
Familial hemophagocytic lymphohistiocytosis (FHL) is one of the most dramatic and life-threatening human inflammatory diseases characterized by prolonged fever, cytopenia, splenomegaly, liver dysfunction, and hemophagocytosis. Most cases of FHL are due to genetic defects in perforin or other genes involved in lymphocyte cytotoxicity. In about 10% of patients with FHL, the genetic basis of the disease remains unresolved.
As a diagnostic reference center, we provide functional immunological evaluation for all HLH patients from German speaking countries. In extension of these diagnostic studies, we characterize the T cell and macrophage response in HLH to better understand the pathophysiological basis of the disease. Patients without a genetic diagnosis are evaluated by whole exome sequencing for novel genetic causes. Patients with HLH offer a unique opportunity to study the molecular regulation of lymphocyte cytotoxicity and intracellular vesicle trafficking. To translate our findings back into clinical application, we have set up an international registry and a clinical study platform for experimental treatment studies on HLH (TREAT-HLH) in collaboration with G. Janka and K. Lehmberg (Hamburg).
We have also established an HLH mouse model based on infection of perforin- or MUNC13-deficient mice with lymphocytic choriomeningitis virus (LCMV) or murine cytomegalovirus (MCMV) to address the following questions:
- Which initial triggers are required for the induction of HLH?
- What is the relevance of persisting antigen for HLH?
- Which cell types and cytokines drive the disease?
Together with Toni Cathomen (CCI), we are using observations in human patients and in MUNC13 deficient mice to prepare gene therapy for human patients with FHL.
Methods
- Flow cytometry
- Functional immune cell analysis
- Signalling studies
- Protein studies
- Fluorescence microscopy
- Cell culture
- Interpretation of genome/exome data
- Genetic manipulation of human T cells
- Mouse models
Cooperations
- Kai Lehmberg, Pädiatrische Hämatologie und Onkologie, Uniklinik Hamburg-Eppendorf
- Peter Aichele, Department für Medizinische Mikrobiologie und Hygiene, Uniklinik Freiburg
- Christoph Schell, Institut für klinische Pathologie, Uniklinik Freiburg
- Toni Cathomen, CCI Freiburg
- Despina Moshous, Institute Imagine, Paris, France
- Claire Booth, Great Ormond Street Hospital, London, UK
- Gillian Griffiths, University of Cambridge, UK
- Yenan Bryceson, Karolinska Institute, Stockholm, Sweden
Funding
- DFG: SFB1160, TP 1 (2015-2019)
Publications
- Patients and mice with deficiency in the SNARE protein SYNTAXIN-11 have a secondary B cell defect. Kögl T, Chang HF, Staniek J, Chiang SCC, Thoulass G, Lao J, Weißert K, Dettmer-Monaco V, Geiger K, Manna PT, Beziat V, Momenilandi M, Tu SM, Keppler SJ, Pattu V, Wolf P, Kupferschmid L, Tholen S, Covill LE, Ebert K, Straub T, Groß M, Gather R, Engel H, Salzer U, Schell C, Maier S, Lehmberg K, Cornu TI, Pircher H, Shahrooei M, Parvaneh N, Elling R, Rizzi M, Bryceson YT, Ehl S, Aichele P, Ammann S. J Exp Med. 2024 Jul 1;221(7):e20221122.
- Survival in primary hemophagocytic lymphohistiocytosis, 2016 to 2021: etoposide is better than its reputation. Böhm S, Wustrau K, Pachlopnik Schmid J, Prader S, Ahlmann M, Yacobovich J, Beier R, Speckmann C, Behnisch W, Ifversen M, Jordan M, Marsh R, Naumann-Bartsch N, Mauz-Körholz C, Hönig M, Schulz A, Malinowska I, Hines M, Nichols KE, Gil-Herrera J, Talano JA, Crooks B, Formankova R, Jorch N, Bakhtiar S, Kühnle I, Streiter M, Nathrath M, Russo A, Dürken M, Lang P, Lindemans C, Henter JI, Lehmberg K, Ehl S. Blood. 2024 Mar 7;143(10):872-881
- Gene editing of hematopoietic stem cells restores T-cell response in familial hemophagocytic lymphohistiocytosis. Dettmer-Monaco V, Weißert K, Ammann S, Monaco G, Lei L, Gräßel L, Rhiel M, Rositzka J, Kaufmann MM, Geiger K, Andrieux G, Lao J, Thoulass G, Schell C, Boerries M, Illert AL, Cornu TI, Ehl S, Aichele P, Cathomen T. J Allergy Clin Immunol. 2024 Jan;153(1):243-255.e14
- Adoptive T cell therapy cures mice from active hemophagocytic lymphohistiocytosis (HLH). Weißert K, Ammann S, Kögl T, Dettmer-Monaco V, Schell C, Cathomen T, Ehl S, Aichele P. EMBO Mol Med. 2022 Dec 7;14(12):e1608
- MAP kinase activating death domain deficiency is a novel cause of impaired lymphocyte cytotoxicity. Schütze K, Groß M, Cornils K, Wustrau K, Schneppenheim S, Lenhartz H, Korenke GC, Janka G, Ledig S, Müller I, Ehl S, Lehmberg K. Blood Adv. 2023 Apr 25;7(8):1531-153
- Rubella vaccine-induced granulomas are a novel phenotype with incomplete penetrance of genetic defects in cytotoxicity. Groß M, Speckmann C, May A, Gajardo-Carrasco T, Wustrau K, Maier SL, Panning M, Huzly D, Agaimy A, Bryceson YT, Choo S, Chow CW, Dückers G, Fasth A, Fraitag S, Gräwe K, Haxelmans S, Holzinger D, Hudowenz O, Hübschen JM, Khurana C, Kienle K, Klifa R, Korn K, Kutzner H, Lämmermann T, Ledig S, Lipsker D, Meeths M, Naumann-Bartsch N, Rascon J, Schänzer A, Seidl M, Tesi B, Vauloup-Fellous C, Vollmer-Kary B, Warnatz K, Wehr C, Neven B, Vargas P, Sepulveda FE, Lehmberg K, Schmitt-Graeff A, Ehl S. J Allergy Clin Immunol. 2022 Jan;149(1):388-399.e4
- NCKAP1L defects lead to a novel syndrome combining immunodeficiency, lymphoproliferation, and hyperinflammation. Castro CN, Rosenzwajg M, Carapito R, Shahrooei M, Konantz M, Khan A, Miao Z, Groß M, Tranchant T, Radosavljevic M, Paul N, Stemmelen T, Pitoiset F, Hirschler A, Nespola B, Molitor A, Rolli V, Pichot A, Faletti LE, Rinaldi B, Friant S, Mednikov M, Karauzum H, Aman MJ, Carapito C, Lengerke C, Ziaee V, Eyaid W, Ehl S*, Alroqi F*, Parvaneh N*, Bahram S*. J Exp Med. 2020 Dec 7;217(12):e2019227
- Neuroinflammatory Disease as an Isolated Manifestation of Hemophagocytic Lymphohistiocytosis. Blincoe A*, Heeg M*, Campbell PK, Hines M, Khojah A, Klein-Gitelman M, Talano JA, Speckmann C, Touzot F, Lankester A, Legger GE, Rivière JG, Garcia-Prat M, Alonso L, Putti MC, Lehmberg K, Maier S, El Chazli Y, Elmaksoud MA, Astigarraga I, Kurjane N, Bulina I, Kenina V, Bryceson Y, Rascon J, Lortie A, Goldstein G, Booth C, Worth A, Wassmer E, Schmitt EG, Warren JT, Bednarski JJ, Ali S, Chiang KY, Krueger J, Henry MM, Holland SM, Marsh RA, Ehl S*, Haddad E*. J Clin Immunol. 2020 Aug;40(6):901-916
- Trigger-dependent differences determine therapeutic outcome in murine primary hemophagocytic lymphohistiocytosis. Gather R, Aichele P, Goos N, Rohr J, Pircher H, Kögl T, Zeiser R, Hengel H, Schmitt-Gräff A, Weaver C, Ehl S. Eur J Immunol. 2020 Nov;50(11):1770-1782
For an up-to-date list of publications by Prof. Stephan Ehl please see the PubMed search.
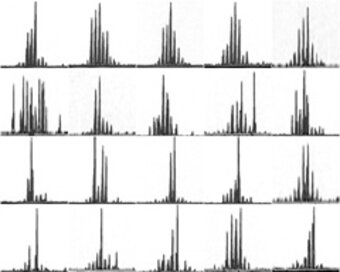
TCR-Spectratyping by P. Fisch
Summary
Combined immunodeficiency (CID) is the phenotypic presentation of a large number of genetic disorders of the immune system. Clinical manifestations include a wide range of infectious diseases including persistent viral and opportunistic infections and manifestations of impaired immune regulation such as autoimmunity, eczema, granulomas or infl ammatory bowel disease. The common immunological abnormality is impaired T cell immunity, but other immune and epithelial cells can also be affected. The study of CID offers a unique opportunity to understand the limiting factors of protective T cell immunity. We approach this problem by the study of individual patients, patient cohorts and mouse models. To transfer this knowledge to patient care, a prospective clinical study has been initiated to better define the threshold when stem cell transplantation should be performed in affected patients.
In the laboratory, we perform a careful phenotypic and functional immunological analysis. In some cases, we identify mutations in known genes and can then analyze the consequence of specific mutations for protein and cellular immune function. In other cases, we use functional assays in combination with exome sequencing to elucidate novel genetic causes for CID. These findings are related to the particular clinical phenotypes with the goal to better understand infection control and immune regulation in humans. We also use mouse models of “leaky” SCID that show features of infection susceptibility and immune dysregulation similar to human patients. In particular, we study T cell development and differentiation and T cell mediated control of viral infections. The overall goal is to understand how human T cell immunity works under limiting conditions.
Methods
- Flow cytometry
- Functional immune cell analysis
- Signalling studies
- Protein studies
- Cell culture
- Interpretation of genome/exome data
- Genetic manipulation of human T cells
- Mouse models
Cooperations
- Wolfgang Schamel, Institute of Biology III, Universität Freiburg
- Despina Moshous, Capucine Picard, Institute Imagine, Paris, France
Funding
- DFG: Euro-CID – Non-SCID combined immunodeficiencies (2016-2019)
Publications
- Long-term robustness of a T-cell system emerging from somatic rescue of a genetic block in T-cell development. Kury P, Führer M, Fuchs S, Lorenz MR, Giorgetti OB, Bakhtiar S, Frei AP, Fisch P, Boehm T, Schwarz K, Speckmann C, Ehl S. EBioMedicine. 2020 Sep;59:102961
- Increased proportions of γδ T lymphocytes in atypical SCID associate with disease manifestations. Tometten I, Felgentreff K, Hönig M, Hauck F, Albert MH, Niehues T, Perez R, Ghosh S, Picard C, Stary J, Formankova R, Worth A, Soler-Palacín P, García-Prat M, Allende LM, Gonzalez-Granado LI, Stepensky P, Di Cesare S, Scarselli A, Cancrini C, Speckmann C, Gilmour K, Notarangelo L, Ehl S, Rohr JC. Clin Immunol. 2019 Apr;201:30-34
- Hemophagocytic lymphohistiocytosis as presenting manifestation of profound combined immunodeficiency due to an ORAI1 mutation. Klemann C, Ammann S, Heizmann M, Fuchs S, Bode SF, Heeg M, Fuchs H, Lehmberg K, Zur Stadt U, Roll C, Vraetz T, Speckmann C, Lorenz MR, Schwarz K, Rohr J, Feske S, Ehl S. J Allergy Clin Immunol. 2017 Dec;140(6):1721-1724
- A prospective study on the natural history of patients with profound combined immunodeficiency: An interim analysis. Speckmann C, Doerken S, Aiuti A, Albert MH, Al-Herz W, Allende LM, Scarselli A, Avcin T, Perez-Becker R, Cancrini C, Cant A, Di Cesare S, Finocchi A, Fischer A, Gaspar HB, Ghosh S, Gennery A, Gilmour K, González-Granado LI, Martinez-Gallo M, Hambleton S, Hauck F, Hoenig M, Moshous D, Neven B, Niehues T, Notarangelo L, Picard C, Rieber N, Schulz A, Schwarz K, Seidel MG, Soler-Palacin P, Stepensky P, Strahm B, Vraetz T, Warnatz K, Winterhalter C, Worth A, Fuchs S, Uhlmann A, Ehl S; P-CID study of the Inborn Errors Working Party of the EBMT. J Allergy Clin Immunol. 2017 Apr;139(4):1302-1310
- Omenn syndrome associated with a functional reversion due to a somatic second-site mutation in CARD11 deficiency. Fuchs S, Rensing-Ehl A, Pannicke U, Lorenz MR, Fisch P, Jeelall Y, Rohr J, Speckmann C, Vraetz T, Farmand S, Schmitt-Graeff A, Krüger M, Strahm B, Henneke P, Enders A, Horikawa K, Goodnow C, Schwarz K, Ehl S. Blood. 2015 Oct 1;126(14):1658-69.
- Deficiency of innate and acquired immunity caused by an IKBKB mutation. Pannicke U, Baumann B, Fuchs S, Henneke P, Rensing-Ehl A, Rizzi M, Janda A, Hese K, Schlesier M, Holzmann K, Borte S, Laux C, Rump EM, Rosenberg A, Zelinski T, Schrezenmeier H, Wirth T, Ehl S*, Schroeder ML*, Schwarz K*. (equal contribution) N Engl J Med. 2013 Dec 26;369(26):2504-14.
- ORAI1-mediated calcium influx is required for human cytotoxic lymphocyte degranulation and target cell lysis. Maul-Pavicic A, Chiang SC, Rensing-Ehl A, Jessen B, Fauriat C, Wood SM, Sjöqvist S, Hufnagel M, Schulze I, Bass T, Schamel WW, Fuchs S, Pircher H, McCarl CA, Mikoshiba K, Schwarz K, Feske S, Bryceson YT, Ehl S. Proc Natl Acad Sci U S A. 2011 Feb 22;108(8):3324-9.
For an up-to-date list of publications by Prof. Stephan Ehl please see the PubMed search.
Summary
The phenotype of benign lymphoproliferation and autoimmunity, in particular autoimmune cytopenia, is observed in a number of primary immunodeficiencies. The most prevalent disorder is autoimmune lymphoproliferative syndrome (ALPS), which is mostly associated with germline or somatic mutations in CD95. CD95 is involved in lymphocyte apoptosis, but has also additional non-apoptotic signaling functions. We investigate the pathophysiological basis of impaired T cell homeostasis in human ALPS by a combination of genetic, phenotypic and functional investigations.
In the last years, new diseases associated with lymphoproliferation and autoimmunity have been discovered. This includes APDS (PIK3CD; PIK3R1), CTLA-4 deficiency or activating mutations in STAT1, STAT3, RAS-pathway associated genes or CARD11 (autosomal-dominant) and LRBA, TPP2, ADA2 or PRKCD deficiency (autosomal-recessive). A number of these conditions affect signalling pathways and metabolic programming of T cells, offering interesting insights into human T cell biology and attractive options for novel therapies.
We have recruited a unique cohort of more than 450 children referred for ALPS evaluation, for which we have clinical data and variable immune phenotyping. While roughly 20% of patients have ALPS and various molecular diagnoses were established in another 30 % of patients, half of the patients remain without genetic diagnosis. Using next generation sequencing, we try to identify new genetic diseases of T cell homeostasis, complemented by in-depth phenotypic and functional immune cell analysis. Candidate genes are validated by appropriate genetic reconstitution experiments and other studies.
Methods
- Flow cytometry
- Functional immune cell analysis
- Cell culture
- RNA seq
- Genetic manipulation of human T cells
- Metabolic studies
Collaborations
- Frederic Rieux-Laucat, Institut Imagine, Paris, France
- Sven Kracker, Institut Imagine, Paris, France
Funding
- DFG: Excellence Cluster CIBSS (2023-2026)
- BMBF: GAIN consortium „Genetic and immunological variability in patients with STAT3 gain-of-function disease.“ (2023-25)
Publications
- Diagnostic evaluation of paediatric autoimmune lymphoproliferative immunodeficiencies (ALPID): a prospective cohort study. Hägele P, Staus P, Scheible R, Uhlmann A, Heeg M, Klemann C, Maccari ME, Ritterbusch H, Armstrong M, Cutcutache I, Elliott KS, von Bernuth H, Leahy TR, Leyh J, Holzinger D, Lehmberg K, Svec P, Masjosthusmann K, Hambleton S, Jakob M, Sparber-Sauer M, Kager L, Puzik A, Wolkewitz M, Lorenz MR, Schwarz K, Speckmann C, Rensing-Ehl A, Ehl S; ALPID study group. Lancet Haematol. 2024 Feb;11(2):e114-e126
- Abnormal biomarkers predict complex FAS or FADD defects missed by exome sequencing. Rensing-Ehl A, Lorenz MR, Führer M, Willenbacher W, Willenbacher E, Sopper S, Abinun M, Maccari ME, König C, Haegele P, Fuchs S, Castro C, Kury P, Pelle O, Klemann C, Heeg M, Thalhammer J, Wegehaupt O, Fischer M, Goldacker S, Schulte B, Biskup S, Chatelain P, Schuster V, Warnatz K, Grimbacher B, Meinhardt A, Holzinger D, Oommen PT, Hinze T, Hebart H, Seeger K, Lehmberg K, Leahy TR, Claviez A, Vieth S, Schilling FH, Fuchs I, Groß M, Rieux-Laucat F, Magerus A, Speckmann C, Schwarz K, Ehl S; ALPS Study Group. J Allergy Clin Immunol. 2024 Jan;153(1):297-308
- Autoimmune lymphoproliferative immunodeficiencies (ALPIDs): A proposed approach to redefining ALPS and other lymphoproliferative immune disorders. Magerus A, Rensing-Ehl A, Rao VK, Teachey DT, Rieux-Laucat F, Ehl S. J Allergy Clin Immunol. 2024 Jan;153(1):67-76
- JAK inhibitor treatment for inborn errors of JAK/STAT signaling: An ESID/EBMT-IEWP retrospective study. Fischer M, Olbrich P, Hadjadj J, Aumann V, Bakhtiar S, Barlogis V, von Bismarck P, Bloomfield M, Booth C, Buddingh EP, Cagdas D, Castelle M, Chan AY, Chandrakasan S, Chetty K, Cougoul P, Crickx E, Dara J, Deyà-Martínez A, Farmand S, Formankova R, Gennery AR, Gonzalez-Granado LI, Hagin D, Hanitsch LG, Hanzlikovà J, Hauck F, Ivorra-Cortés J, Kisand K, Kiykim A, Körholz J, Leahy TR, van Montfrans J, Nademi Z, Nelken B, Parikh S, Plado S, Ramakers J, Redlich A, Rieux-Laucat F, Rivière JG, Rodina Y, Júnior PR, Salou S, Schuetz C, Shcherbina A, Slatter MA, Touzot F, Unal E, Lankester AC, Burns S, Seppänen MRJ, Neth O, Albert MH, Ehl S, Neven B, Speckmann C. J Allergy Clin Immunol. 2024 Jan;153(1):275-286.e18
- Combined germline and somatic human FADD mutations cause autoimmune lymphoproliferative syndrome. Pellé O, Moreno S, Lorenz MR, Riller Q, Fuehrer M, Stolzenberg MC, Maccari ME, Lenoir C, Cheminant M, Hinze T, Hebart HF, König C, Schvartz A, Schmitt Y, Vinit A, Henry E, Touzart A, Villarese P, Isnard P, Neveux N, Landman-Parker J, Picard C, Fouyssac F, Neven B, Grimbacher B, Speckmann C, Fischer A, Latour S, Schwarz K, Ehl S, Rieux-Laucat F, Rensing-Ehl A, Magérus A. J Allergy Clin Immunol. 2024 Jan;153(1):203-21
- Activated phosphoinositide 3-kinase δ syndrome: Update from the ESID Registry and comparison with other autoimmune-lymphoproliferative inborn errors of immunity. Maccari ME, Wolkewitz M, … Ehl, S. J Allergy Clin Immunol. 2023 Oct;152(4):984-996.e10
- Revisiting autoimmune lymphoproliferative syndrome caused by Fas ligand mutations. Maccari ME, Schneider P, Smulski CR, Meinhardt A, Pinto F, Gonzalez-Granado LI, Schuetz C, Sica MP, Gross M, Fuchs I, Kury P, Heeg M, Vocat T, Willen L, Thomas C, Hühn R, Magerus A, Lorenz M, Schwarz K, Rieux-Laucat F, Ehl S, Rensing-Ehl A. J Allergy Clin Immunol. 2023 May;151(5):1391-1401
- STAT3-confusion-of-function: Beyond the loss and gain dualism. Lodi L, Faletti LE, Maccari ME, Consonni F, Groß M, Pagnini I, Ricci S, Heeg M, Simonini G, Azzari C, Ehl S. J Allergy Clin Immunol. 2022 Nov;150(5):1237-1241
For an up-to-date list of publications by Prof. Stephan Ehl please see the PubMed search.
Collaborations
- Dr. Peter Aichele, Institute for Immunodeficiency, Medical Center - University of Freiburg
- Prof. Marta Rizzi, Department of Rheumatology and Clinical Immunology, Medical Center - University of Freiburg
- Prof. Tomas Kalina, Faculty of Medicine, Charles University Prague
- Prof. Herve Luche, CIPHE Department, University Marseille
- Prof. Dr. Toni Cathomen, Institute for Transfusion Medicine and Gene Therapy, Medical Center - University of Freiburg
- Prof. Dr. Frederic Rieux-Laucat, Institute Imagine, Paris
- Prof. Dr. Aude Magerus, Institute Imagine, Paris
Publications
HLH
Wegehaupt, O., O. Borisov, E. Sieni, F. Oyen, J. Mann, M.L. Coniglio, A.P. Chinnici, F. Pegoraro, L. Beneforti, K.C. Gilmour, D. Moshous, G. de Saint Basile, W. Zhang, R.A. Marsh, C. De Fusco, K. Wustrau, F. Timeus, C. Micalizzi, E. Gunsilius, L. Hosking, S. Choo, S. Ghosh, A. Kottgen, K. Lehmberg, and S. Ehl. 2025. Beyond genotype: challenges in predicting disease risk for carriers of biallelic perforin variants. Blood doi:10.1182/blood.2024027954.
Mann, J., S. Runge, C. Schell, K. Grawe, G. Thoulass, J. Lao, S. Ammann, S. Grun, C. Konig, S.A. Berger, B. Hild, P. Aichele, S.P. Rosshart, and S. Ehl. 2025. The Microbiome Modifies Manifestations of Hemophagocytic Lymphohistiocytosis in Perforin-Deficient Mice. Eur J Immunol 55:e202451061. doi:10.1002/eji.202451061.
Bohm, S., K. Wustrau, J. Pachlopnik Schmid, S. Prader, M. Ahlmann, J. Yacobovich, R. Beier, C. Speckmann, W. Behnisch, M. Ifversen, M. Jordan, R. Marsh, N. Naumann-Bartsch, C. Mauz-Korholz, M. Honig, A. Schulz, I. Malinowska, M. Hines, K.E. Nichols, J. Gil-Herrera, J.A. Talano, B. Crooks, R. Formankova, N. Jorch, S. Bakhtiar, I. Kuhnle, M. Streiter, M. Nathrath, A. Russo, M. Durken, P. Lang, C. Lindemans, J.I. Henter, K. Lehmberg, and S. Ehl. 2024. Survival in primary hemophagocytic lymphohistiocytosis, 2016 to 2021: etoposide is better than its reputation. Blood 143:872-881. doi:10.1182/blood.2023022281.
Schutze, K.*, M. Gross*, K. Cornils, K. Wustrau, S. Schneppenheim, H. Lenhartz, G.C. Korenke, G. Janka, S. Ledig, I. Muller, S. Ehl, and K. Lehmberg. 2023. MAP kinase activating death domain deficiency is a novel cause of impaired lymphocyte cytotoxicity. Blood Adv 7:1531-1535. doi:10.1182/bloodadvances.2022008195.
Weissert, K., S. Ammann, T. Kogl, V. Dettmer-Monaco, C. Schell, T. Cathomen, S. Ehl, and P. Aichele. 2022. Adoptive T cell therapy cures mice from active hemophagocytic lymphohistiocytosis (HLH). EMBO Mol Med 14:e16085. doi:10.15252/emmm.202216085.
Gross, M., C. Speckmann, A. May, T. Gajardo-Carrasco, K. Wustrau, S.L. Maier, M. Panning, D. Huzly, A. Agaimy, Y.T. Bryceson, S. Choo, C.W. Chow, G. Duckers, A. Fasth, S. Fraitag, K. Grawe, S. Haxelmans, D. Holzinger, O. Hudowenz, J.M. Hubschen, C. Khurana, K. Kienle, R. Klifa, K. Korn, H. Kutzner, T. Lammermann, S. Ledig, D. Lipsker, M. Meeths, N. Naumann-Bartsch, J. Rascon, A. Schanzer, M. Seidl, B. Tesi, C. Vauloup-Fellous, B. Vollmer-Kary, K. Warnatz, C. Wehr, B. Neven, P. Vargas, F.E. Sepulveda, K. Lehmberg, A. Schmitt-Graeff, and S. Ehl. 2022. Rubella vaccine-induced granulomas are a novel phenotype with incomplete penetrance of genetic defects in cytotoxicity. J Allergy Clin Immunol 149:388-399 e384. doi:10.1016/j.jaci.2021.05.007.
Castro, C.N.*, M. Rosenzwajg*, R. Carapito*, M. Shahrooei*, M. Konantz, A. Khan, Z. Miao, M. Gross, T. Tranchant, M. Radosavljevic, N. Paul, T. Stemmelen, F. Pitoiset, A. Hirschler, B. Nespola, A. Molitor, V. Rolli, A. Pichot, L.E. Faletti, B. Rinaldi, S. Friant, M. Mednikov, H. Karauzum, M.J. Aman, C. Carapito, C. Lengerke, V. Ziaee, W. Eyaid, S. Ehl*, F. Alroqi*, N. Parvaneh*, and S. Bahram*. 2020. NCKAP1L defects lead to a novel syndrome combining immunodeficiency, lymphoproliferation, and hyperinflammation. J Exp Med 217:doi:10.1084/jem.20192275.
*equal contribution
P-CID
Kury, P., M. Fuhrer, S. Fuchs, M.R. Lorenz, O.B. Giorgetti, S. Bakhtiar, A.P. Frei, P. Fisch, T. Boehm, K. Schwarz, C. Speckmann, and S. Ehl. 2020. Long-term robustness of a T-cell system emerging from somatic rescue of a genetic block in T-cell development. EBioMedicine 59:102961. doi:10.1016/j.ebiom.2020.102961.
Speckmann, C., S. Doerken, A. Aiuti, M.H. Albert, W. Al-Herz, L.M. Allende, A. Scarselli, T. Avcin, R. Perez-Becker, C. Cancrini, A. Cant, S. Di Cesare, A. Finocchi, A. Fischer, H.B. Gaspar, S. Ghosh, A. Gennery, K. Gilmour, L.I. Gonzalez-Granado, M. Martinez-Gallo, S. Hambleton, F. Hauck, M. Hoenig, D. Moshous, B. Neven, T. Niehues, L. Notarangelo, C. Picard, N. Rieber, A. Schulz, K. Schwarz, M.G. Seidel, P. Soler-Palacin, P. Stepensky, B. Strahm, T. Vraetz, K. Warnatz, C. Winterhalter, A. Worth, S. Fuchs, A. Uhlmann, S. Ehl, and P.C.s.o.t.I.E.W.P.o.t. EBMT. 2017. A prospective study on the natural history of patients with profound combined immunodeficiency: An interim analysis. J Allergy Clin Immunol 139:1302-1310 e1304. doi:10.1016/j.jaci.2016.07.040.
AL-PID
Hadjadj, J., A. Wolfers, O. Borisov, D. Hazard, R. Leahy, M. Jeanpierre, A. Belot, S. Bakhtiar, F. Hauck, P.Y. Lee, S. Volpi, S. Palmeri, V. Barlogis, N. Aladjidi, G. Ebetsberger-Dachs, J. Avouac, F. Charbit-Henrion, M. Cheminant, J. Donadieu, S. Ghosh, D.P. Hoytema van Konijnenburg, J. Korholz, J. Bustamante, J. Rosain, L. Forbes Satter, I. Selmeryd, G. Sogkas, B. Neven, F. Rieux-Laucat, S. Ehl, and S.S. Group. 2025. Clinical manifestations, disease penetrance, and treatment in individuals with SOCS1 insufficiency: a registry-based and population-based study. Lancet Rheumatol doi:10.1016/S2665-9913(24)00348-5.
Rensing-Ehl, A., M.R. Lorenz, M. Fuhrer, W. Willenbacher, E. Willenbacher, S. Sopper, M. Abinun, M.E. Maccari, C. Konig, P. Haegele, S. Fuchs, C. Castro, P. Kury, O. Pelle, C. Klemann, M. Heeg, J. Thalhammer, O. Wegehaupt, M. Fischer, S. Goldacker, B. Schulte, S. Biskup, P. Chatelain, V. Schuster, K. Warnatz, B. Grimbacher, A. Meinhardt, D. Holzinger, P.T. Oommen, T. Hinze, H. Hebart, K. Seeger, K. Lehmberg, T.R. Leahy, A. Claviez, S. Vieth, F.H. Schilling, I. Fuchs, M. Gross, F. Rieux-Laucat, A. Magerus, C. Speckmann, K. Schwarz, S. Ehl, and A.S. Group. 2024. Abnormal biomarkers predict complex FAS or FADD defects missed by exome sequencing. J Allergy Clin Immunol 153:297-308 e212. doi:10.1016/j.jaci.2023.11.006.
Pelle, O.*, S. Moreno*, M.R. Lorenz*, Q. Riller, M. Fuehrer, M.C. Stolzenberg, M.E. Maccari, C. Lenoir, M. Cheminant, T. Hinze, H.F. Hebart, C. Konig, A. Schvartz, Y. Schmitt, A. Vinit, E. Henry, A. Touzart, P. Villarese, P. Isnard, N. Neveux, J. Landman-Parker, C. Picard, F. Fouyssac, B. Neven, B. Grimbacher, C. Speckmann, A. Fischer, S. Latour, K. Schwarz, S. Ehl*, F. Rieux-Laucat*, A. Rensing-Ehl*, and A. Magerus*. 2024. Combined germline and somatic human FADD mutations cause autoimmune lymphoproliferative syndrome. J Allergy Clin Immunol 153:203-215. doi:10.1016/j.jaci.2023.09.028.
Hagele, P., P. Staus, R. Scheible, A. Uhlmann, M. Heeg, C. Klemann, M.E. Maccari, H. Ritterbusch, M. Armstrong, I. Cutcutache, K.S. Elliott, H. von Bernuth, T.R. Leahy, J. Leyh, D. Holzinger, K. Lehmberg, P. Svec, K. Masjosthusmann, S. Hambleton, M. Jakob, M. Sparber-Sauer, L. Kager, A. Puzik, M. Wolkewitz, M.R. Lorenz, K. Schwarz, C. Speckmann, A. Rensing-Ehl, S. Ehl, and A.s. group. 2024. Diagnostic evaluation of paediatric autoimmune lymphoproliferative immunodeficiencies (ALPID): a prospective cohort study. Lancet Haematol 11:e114-e126. doi:10.1016/S2352-3026(23)00362-9.
Maccari, M.E.*, S. Fuchs*, P. Kury*, G. Andrieux, S. Volkl, B. Bengsch, M.R. Lorenz, M. Heeg, J. Rohr, S. Jagle, C.N. Castro, M. Gross, U. Warthorst, C. Konig, I. Fuchs, C. Speckmann, J. Thalhammer, F.G. Kapp, M.G. Seidel, G. Duckers, S. Schonberger, C. Schutz, M. Fuhrer, R. Kobbe, D. Holzinger, C. Klemann, P. Smisek, S. Owens, G. Horneff, R. Kolb, N. Naumann-Bartsch, M. Miano, J. Staniek, M. Rizzi, T. Kalina, P. Schneider, A. Erxleben, R. Backofen, A. Ekici, C.M. Niemeyer, K. Warnatz, B. Grimbacher, H. Eibel, A. Mackensen, A.P. Frei, K. Schwarz, M. Boerries, S. Ehl*, and A. Rensing-Ehl*. 2021. A distinct CD38+CD45RA+ population of CD4+, CD8+, and double-negative T cells is controlled by FAS. J Exp Med 218:doi:10.1084/jem.20192191.
Hadjadj, J.*, C.N. Castro*, M. Tusseau, M.C. Stolzenberg, F. Mazerolles, N. Aladjidi, M. Armstrong, H. Ashrafian, I. Cutcutache, G. Ebetsberger-Dachs, K.S. Elliott, I. Durieu, N. Fabien, M. Fusaro, M. Heeg, Y. Schmitt, M. Bras, J.C. Knight, J.C. Lega, G. Lesca, A.L. Mathieu, M. Moreews, B. Moreira, A. Nosbaum, M. Page, C. Picard, T. Ronan Leahy, I. Rouvet, E. Ryan, D. Sanlaville, K. Schwarz, A. Skelton, J.F. Viallard, S. Viel, M. Villard, I. Callebaut, C. Picard, T. Walzer, S. Ehl, A. Fischer, B. Neven, A. Belot, and F. Rieux-Laucat. 2020. Early-onset autoimmunity associated with SOCS1 haploinsufficiency. Nat Commun 11:5341. doi:10.1038/s41467-020-18925-4.
*equal contribution
Team

Prof. Dr. med. Stephan Ehl
MEDICAL CENTER - UNIVERSITY OF FREIBURG
Center for Chronic Immunodeficiency
at Center for Translational Cell Research
Breisacher Str. 115
79106 Freiburg
Germany
Phone: +49 (0)761 270-77550 (Secretary)
Fax: +49 (0)761 270-77600
stephan.ehl@uniklinik-freiburg.de

